Iron Overload and PCOS #35
What is the link between PCOS and Iron Overload?
Hello lovely people,
How was your week? I am writing to you today from beautiful Malta. We are here for three weeks with my partner’s family. Look at this beauty 👇🏼.
Today I want to touch on an interesting piece of the puzzle for my PCOS: iron. The more I deepen my knowledge of this condition, the more I understand what happened to me and why I have PCOS.
This week’s question
What is the link between PCOS and Iron Overload?
Before we get into the connection between the two, let’s quickly revise what Iron is and what it does in the body.
Iron is a mineral naturally present in many foods, added to some food products, and available as a dietary supplement. Iron is an essential component of haemoglobin - a key protein that transfers oxygen from the lungs to the tissues. Due to its important job in the body, iron is a mineral we always need to watch.
How does it link to PCOS?
Several proteins connected to the biology of iron are altered in blood in patients with PCOS, and most of these changes suggest a mild iron overload in women with PCOS. Whilst most women will experience low Iron levels, we might see the opposite on a blood test result.
Why is having too much Iron in the blood problematic?
Even though iron is an essential element for cell survival, it is highly oxidative capable of generating reactive oxygen species (ROS). ROS are unstable molecules in the body that can create inflammation and damage our organs. Think about how iron poles turn rusty over time. This is because oxygen from our atmosphere interacts with the iron particle on the pole, damaging it. However, iron overload in women with PCOS is mild, so we shouldn’t be scared.
This newsletter will remain free as I believe access to research and information shouldn’t have barriers. However, if you’d like to support my writing for the cost of a coffee per month, I would appreciate it. I dedicate most of my weekends and free time to this project, and your support will mean the world to me.
Why is there more iron than needed?
Recent findings show that women with PCOS display lower levels of Hepcidin, a hormone that regulates iron levels in the blood. These low levels promote higher levels of iron. Excess insulin and excess testosterone are thought to promote these levels.
In addition, there is also a specific genetic mutation that can lead to this overload and ultimately to a condition called Haemochromatosis.
Haemochromatosis is an inherited condition where iron levels in the body slowly build up over many years due to a genetic mutation within the HFE gene. Guess what? I have the mutation 👇🏼.
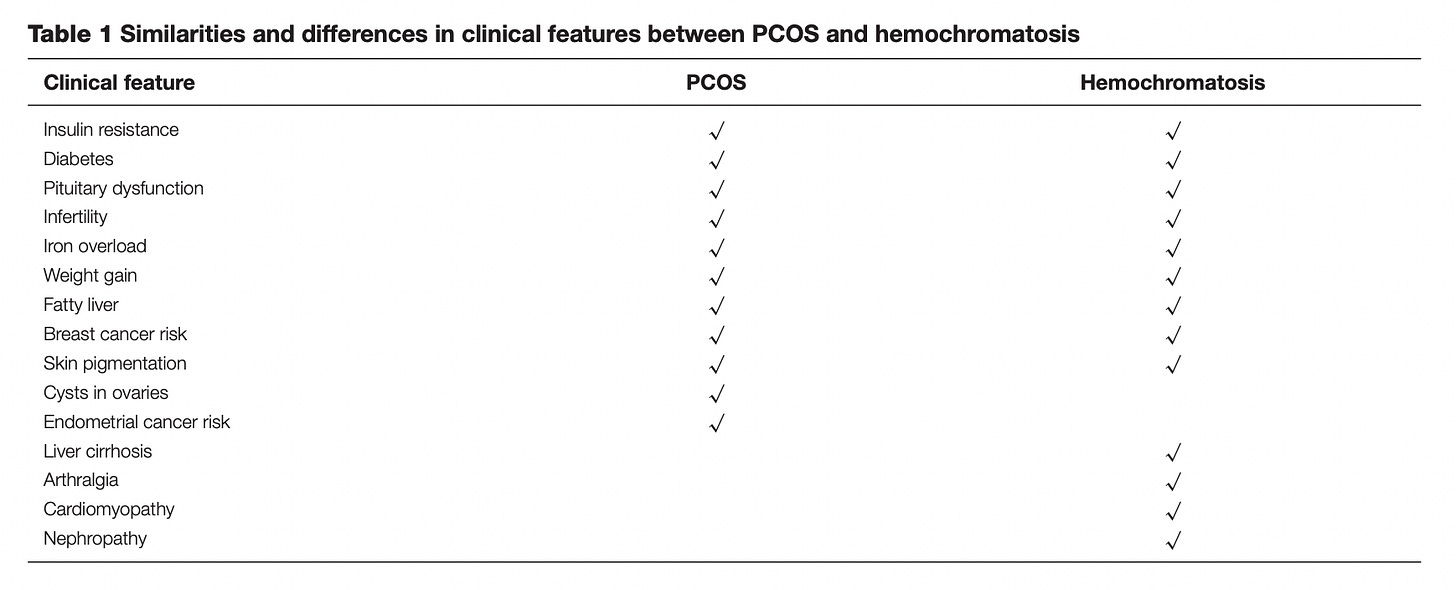
Hemochromatosis shares a lot of common symptoms with PCOS (as you see in the image below), so I am now asking myself, is this mutation what is causing my PCOS-like symptoms?
However, a difference between the two disorders is that the clinical symptoms in PCOS appear at a much younger age. In contrast, they become evident in Hemochromatosis at a much later age. Given that I have had issues with my period since I was 12, maybe it is not only this mutation that is causing me issues.
It doesn’t seem to be a direct causative link in research, but I am happy to have discovered another potential explanation for why I have PCOS. Getting to know my body and investigating what is happening brings me much peace. I think this is an evaluation of medicine that puts the patient in control of their health, and I believe is right for us to be our main advocate.
I hope you enjoyed reading this newsletter.
See you next Sunday,
Francesca
1 Sources
Luque-Ramírez, M., Álvarez-Blasco, F., Alpañés, M., & Escobar-Morreale, H. F. (2011). Role of decreased circulating hepcidin concentrations in the iron excess of women with the polycystic ovary syndrome. The Journal of Clinical Endocrinology and Metabolism, 96(3), 846–852. https://doi.org/10.1210/jc.2010-2211
Mathew, M., Sivaprakasam, S., Phy, J. L., Bhutia, Y. D., & Ganapathy, V. (2023). Polycystic ovary syndrome and iron overload: biochemical link and underlying mechanisms with potential novel therapeutic avenues. Bioscience Reports, 43(1). https://doi.org/10.1042/BSR20212234
Disclaimer: We are all unique in our ways, so this information is for educational purposes only. In my communications, I summarise research data and bring my experience. This shouldn’t be viewed as medical advice at any point. Please further consult your healthcare provider about your health needs.